The Algorithm That Sees What Doctors Miss
AI diagnostics are rewriting the rules of radiology — detecting cancers earlier, faster, and with startling accuracy that is challenging human expertise.
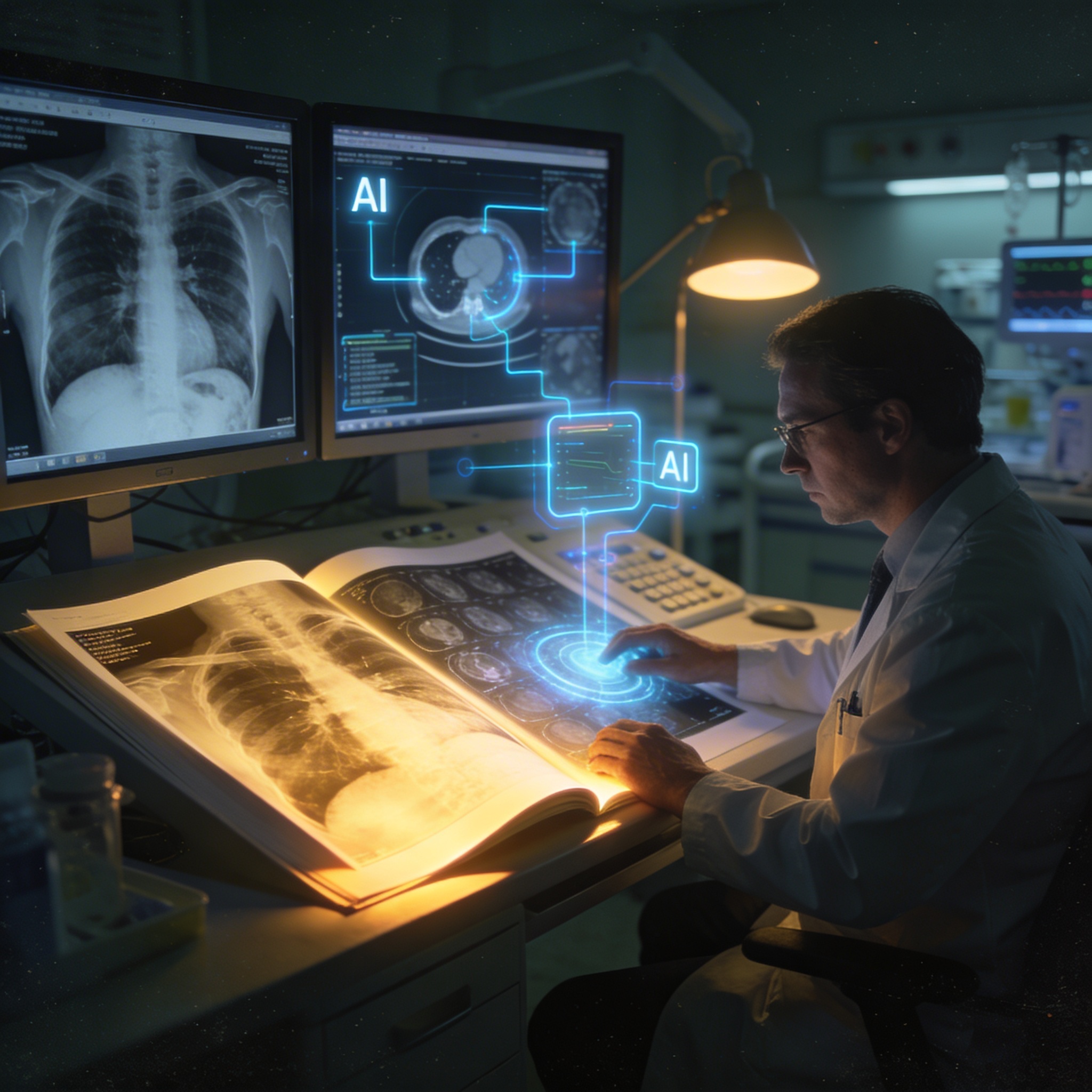
Picture a radiologist staring at a chest scan at 11 p.m., her fourth hour of back-to-back image reads, fatigue quietly dulling the sharp instincts that years of training built. Now picture an algorithm that never tires, never blinks, and has studied more scans in a single training cycle than most physicians will see in a lifetime. That contrast — human limitation versus machine endurance — sits at the center of one of medicine's most consequential debates. In 2026, artificial intelligence is no longer knocking at radiology's door. It has walked in, sat down, and started outperforming the experts.
Picture a radiologist staring at a chest scan at 11 p.m., her fourth hour of back-to-back image reads, fatigue quietly dulling the sharp instincts that years of training built. Now picture an algorithm that never tires, never blinks, and has studied more scans in a single training cycle than most physicians will see in a lifetime. That contrast — human limitation versus machine endurance — sits at the center of one of medicine's most consequential debates. In 2026, artificial intelligence is no longer knocking at radiology's door. It has walked in, sat down, and started outperforming the experts.
The Numbers Don't Lie — AI Is Getting It Right
The statistics arriving from research institutions and hospital systems are difficult to dismiss. AI-powered medical imaging tools are now demonstrating a 17.6% higher cancer detection rate compared to traditional human-only interpretation methods, according to reporting from Articsledge [1]. That figure is not a rounding error or a laboratory curiosity. It represents real tumors caught earlier, real patients who will survive because a machine flagged something a tired human eye might have skimmed past at the end of a grueling shift.
In one of the most striking examples, an AI system evaluated by Scispot achieved a 94% accuracy rate in detecting lung nodules — a result that significantly outpaced the performance of human radiologists working under standard clinical conditions [10]. Lung cancer, which kills more people globally than any other cancer, depends on early detection for survivability. A system that finds nodules at that rate of accuracy is not a novelty tool. It is a clinical necessity.
Peer-reviewed validation has been building steadily. A systematic review and meta-analysis published in *Nature* examined 83 studies and found that AI models performed on par with — and in several key domains, exceeded — physician-level diagnostic accuracy [8]. The MDPI journal *Diagnostics* similarly confirmed that AI tools have materially enhanced diagnostic accuracy and efficiency in detecting abnormalities across multiple imaging modalities, including CT, MRI, and mammography, through automated feature extraction that human readers simply cannot replicate at scale [6].
iCAD's ProFound AI system offers a concrete case study. Peer-reviewed research confirmed that the platform significantly increases cancer detection rates in mammography and boosts overall diagnostic accuracy, reducing the number of false positives that send patients spiraling into unnecessary follow-up procedures and anxiety [5]. In stroke care, the speed advantage is equally dramatic. AI triage systems are now accelerating treatment decisions in acute stroke cases, shaving critical minutes off door-to-needle times in a condition where every 60 seconds of delay destroys nearly two million neurons [1]. The machines are not just matching human performance. In measurable, reproducible ways, they are beginning to surpass it.
---
""In some settings, AI is already surpassing doctors — and the lead will only widen.""
The Human Factor — Where the Algorithm Complicates the Picture

Not every radiologist who picks up an AI-assisted workflow emerges a better diagnostician. This is one of the more uncomfortable findings to surface from recent research, and it deserves serious attention rather than convenient dismissal. A study from Harvard Medical School found that while AI tools improve diagnostic performance for some radiologists, they actively worsen outcomes for others [2]. The variable is not the algorithm. It is the human operating alongside it.
The phenomenon has a name in cognitive science: automation bias. When a confident AI system flags a scan as clear, some physicians reduce their own scrutiny, trusting the machine more than their trained instincts. The result can be a missed finding — one that the radiologist, working independently, might have caught. Cardiologist and researcher Dr. Eric Topol, one of the most respected voices on AI in medicine, has documented a series of recent studies comparing the performance of doctors working with AI versus AI systems operating alone. The findings were jarring: in several scenarios, AI alone outperformed the doctor-AI combination [3].
This does not mean collaboration is worthless. It means the collaboration must be designed carefully, with radiologists trained not merely to use AI tools but to interrogate them. The question of transparency has become urgent in 2026. The Imaging Wire's analysis of top radiology trends this year raised a pointed issue: should radiologists be required to disclose when they use AI to interpret medical images, and if so, how exactly should that disclosure work [9]? Patients, insurers, and hospital systems are all beginning to ask the same question.
The liability architecture has not kept pace with the technology. As Radiology Business reported in 2026, AI is not foolproof and can contribute to diagnostic mistakes for which radiologists — not the algorithm's developers — can be held legally responsible [radiologybusiness.com]. That asymmetry, where a machine makes the error but a human carries the consequence, is generating friction across the specialty and forcing professional bodies to rethink how accountability is assigned in an AI-assisted clinical environment. The era of easy answers ended the moment these tools became good enough to matter.
---
""An AI system that reads a chest X-ray in seconds may be the only radiologist a patient in rural Kenya ever encounters.""
Speed, Scale, and the Global Access Argument
Beyond raw accuracy, AI's most transformative contribution to radiology may be one that gets far less attention in the headline-grabbing performance comparisons: sheer scale. The global shortage of trained radiologists is severe, particularly in sub-Saharan Africa, rural South Asia, and underserved regions of Latin America, where imaging equipment exists but the expertise to interpret results often does not. The World Economic Forum has documented how AI is beginning to address this gap, enabling diagnostic-quality image interpretation in settings where no specialist would otherwise be available [13].
An AI system that can read a chest X-ray in seconds and flag abnormalities with clinical-grade accuracy is not replacing a radiologist in a well-staffed urban hospital. In a district clinic in rural Kenya or a community health center in rural Montana, it may be the only radiologist the patient ever encounters. That reframing matters enormously when evaluating the technology's net impact on human health.
Speed, too, operates as a patient safety variable in ways that pure accuracy metrics cannot fully capture. A 2025 report from Chase Lodge Hospital noted that AI diagnostic platforms are dramatically compressing the time between image acquisition and actionable clinical insight [7], a compression that has measurable consequences in oncology, neurology, and emergency medicine. The average number of AI use cases per physician rose from 1.1 in 2023 to 2.3 in 2026, according to data reported by AuntMinnie [auntminnie.com], a signal that adoption is accelerating beyond early adopters and into mainstream clinical practice.
Diagnostic Imaging's analysis of radiology's inflection point in 2026 put it plainly: the field now needs AI tools that can synthesize findings, summarize prior exams, factor in clinician intent, and translate raw image data into genuinely actionable recommendations [12]. The technology is moving from pattern recognition to clinical reasoning — a transition that narrows the gap between what machines do and what physicians have long believed only they could do.
---

""The machines are extraordinary. They are also, still, tools — and the hands that wield them remain the most important variable in the room.""
The Future Belongs to the Partnership, Not the Machine Alone
The most intellectually honest position in 2026 is this: AI is outperforming human radiologists in specific, well-defined tasks, and that lead will widen. But the version of the future where algorithms replace physicians entirely remains, for now, a misreading of both the technology and the clinical environment it operates within. CNN's reporting on radiology as a case study in AI's job-displacement narrative found that today's radiologists are deploying AI to prioritize scan queues, enhance image quality, and accelerate report summaries — augmenting their workflow rather than being erased by it [cnn.com].
TIME Magazine's healthcare AI analysis, drawing on Dr. Topol's extensive research, framed the honest duality well: in some settings, AI is already surpassing doctors; in others, it fails in ways that are difficult to predict and sometimes dangerous [time.com]. The task for the specialty is not to choose between human expertise and machine intelligence but to build systems sophisticated enough to leverage both without allowing either to cover for the other's blind spots.
Indiana University's School of Medicine has positioned radiology as a leader in responsible AI adoption, emphasizing that the training of future radiologists must include not just technical fluency with AI tools but critical evaluation of their outputs [23]. The Radiological Society of North America echoed this in its 2025 guidance, noting that AI's role in medical imaging must be understood as a dynamic collaboration rather than a static handoff [24].
What is already beyond debate is that the diagnostic landscape has changed permanently. The question facing hospital administrators, training programs, residency directors, and practicing radiologists is not whether to integrate AI but how to do it without surrendering the clinical judgment that no algorithm, however sophisticated, has yet managed to fully replicate. The machines are extraordinary. They are also, still, tools — and the hands that wield them remain the most important variable in the room.
The future of radiology will not be written by the algorithm that sees the most. It will be written by the physician wise enough to know what the algorithm missed.
---

